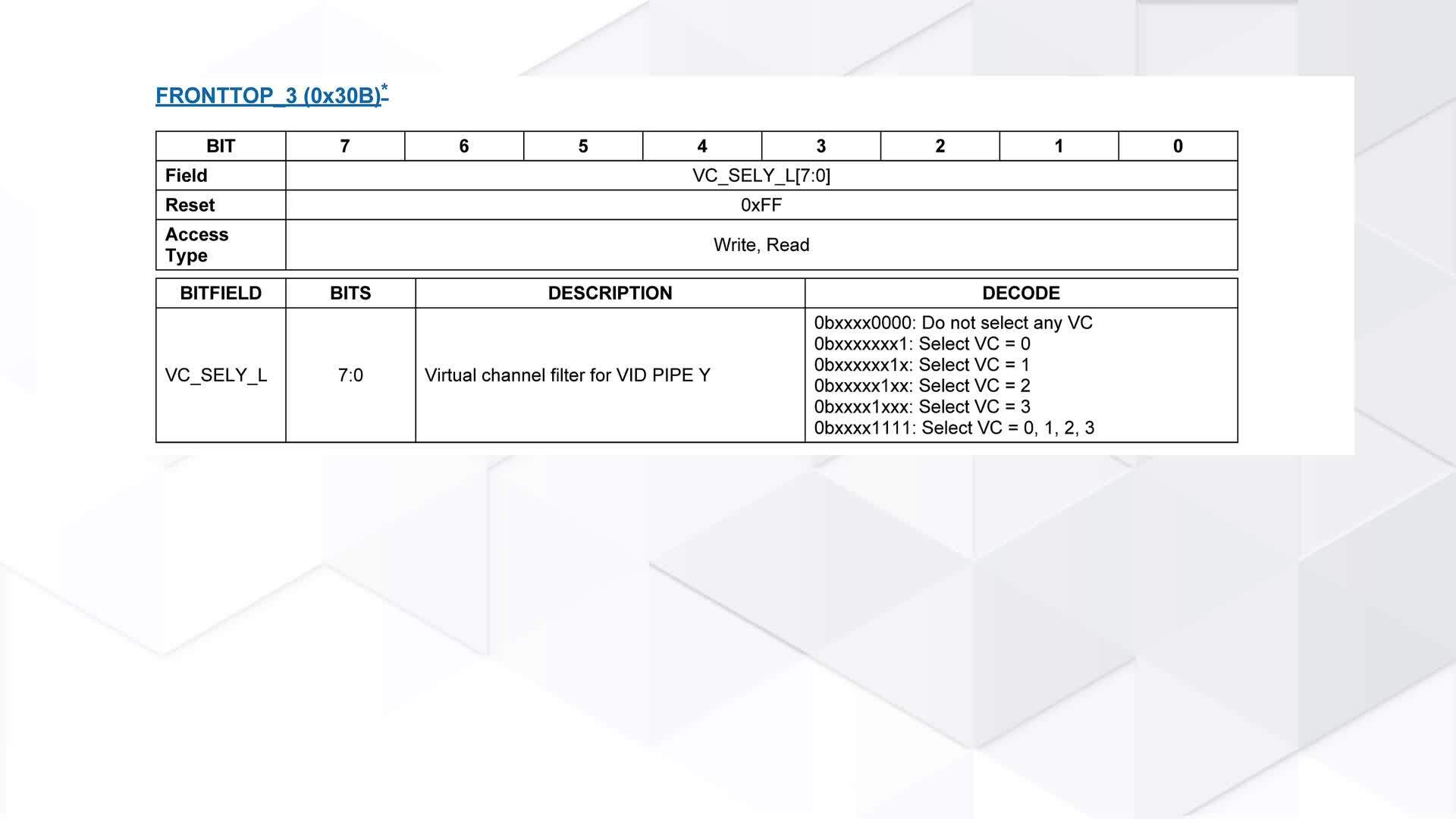
要約
This tutorial provides an introduction to dialysis machines and discusses FDA regulation and IEC 60601-1 certification, self-test and fault-indication capabilities, form-factor requirements, power-budget constraints, and other critical design considerations. It describes the main subfunctions of dialysis systems—including the extracorporeal, dialysate, and disinfection circuits—as well as component selection criteria for the display, data interface, sensing and mechanics, processing, and power.
Overview

Clinical dialysis machine
Dialysis machines are artificial kidneys that perform most, but not all, kidney functions for patients who have permanent or temporary renal failure. The machines use hemodialysis to cleanse the blood and balance its constituents. With this process, the patient's blood is circulated through the machine where it is filtered and balanced for electrolytes, pH, and fluid concentration before being returned to the patient. One common problem with renal failure is water retention, so it is common for the process to remove several pints of fluid from the patient's blood.
There are two basic classes of dialysis machines: clinical units, which are commonly cabinet-size machines operated by trained technicians; and home-use dialysis machines, which are smaller and sometimes portable.
Normally, patients with complete loss of kidney function would need to visit the clinic at least three times per week and spend about four hours connected to the machine. With home-use machines, patients have more flexibility in scheduling dialysis, and they can dialyze for longer periods and more frequently. Thus, home-use machines are growing in popularity because they offer greater convenience and better clinical outcomes.
FDA-Regulated Medical Equipment
Dialysis machines are medical equipment whose design and manufacture is regulated by the Food and Drug Administration (FDA). This means that their design and construction must follow precisely documented processes, and their performance must meet stringent documentation, development testing, production testing, and field maintenance requirements.
The equipment also must contain comprehensive self-test and fault-indication capabilities, which require additional circuitry and the use of components that include self-test features.
Electrical leakage to the patient is a significant concern. Medical device developers must meet the requirements of the IEC 60601-1 product safety standard for electrical medical equipment.
Given the time and expense required to achieve FDA approval, manufacturers must ensure the long-term availability of system components. Thus, it is important to select a supplier with a customer-oriented discontinuance policy to ensure that system components will be available for many years.
Medical customers rely on Maxim products because over the years we have carefully avoided discontinuing parts. We realize how devastating product discontinuance can be to a customer, so we work diligently to transfer some products to newer production lines, create wafer buffers, allow last-time purchases, or develop upgrade devices. Very few Maxim parts have ever been discontinued while demand still existed. Maxim's Discontinuance Policy is one of the most flexible among our peer supplier companies.
General Operation
Extracorporeal Circuit
The patient's blood is continuously pumped from an artery, a large vein, or a surgically modified vein to allow high blood flow rates. Its pressure is monitored both upstream and downs-tream from the peristaltic blood pump. Before the blood enters the dialyzer, heparin is added to prevent clotting. A syringe pump is used to deliver the heparin at a precisely controlled rate.
The blood then enters the dialyzer where it passes across a large-surface-area, semipermeable membrane with a dialysate solution on the other side. A pressure gradient is maintained across the membrane to ensure the proper flow of compounds out of and into the blood. After cleansing and balancing within the dialyzer, the blood is passed through an air trap to remove any air bubbles before it is returned to the patient. An air bubble sensor ensures that no air bubbles remain.
Blood-pressure, oxygen-saturation, and sometimes hematocrit levels (blood cell concentration) are monitored for proper operation of the machine and to ensure patient safety. For maximum effectiveness, fresh dialysate is continually pumped through the dialyzer during operation.
Dialysate Circuit
In clinical settings, dialysate is usually premixed to the proper concentration for direct use. In home units, to keep container size down, concentrated forms of dialysate are often used and diluted with sterilized water in the machine. Thus, home units must include water heaters, valves, pumps, and a variety of sensors to perform these extra steps. To lower power consumption in home units, the dialysate preparation process is often performed ahead of time, separately from dialysis.
Both types of machines include capabilities to add a bicarbonate buffer solution to the dialysate. This subcircuit comprises additional pumps, valves, and sensors.
Disinfection Circuit
After the dialysis procedure, the machine must be cleansed and sterilized. Provisions are made in the plumbing to close the circuit into a loop and run saline and/or sterilized water through the system to flush away all impurities.
Special Requirements of Home Units
For general convenience, home systems are smaller and sometimes portable. Since they require the additional function of dialysate preparation, the need for small, compact design is increased over clinical machines.
Low power draw is also important in home dialysis units. Earlier systems often required home rewiring to allow more than the typical 15A capability of a 110V AC branch circuit. Today, low-power design can eliminate the need for these costly modifications.
The disinfection cycle at the end of therapy is also a power-hungry process. To accomplish the heating required in a reasonable amount of time, batteries or ultracapacitors are included to provide short-term high-power capability to supplement line power as needed. When line-power usage drops below the 15A limit, the batteries or ultracapacitors are recharged.

Block diagram of a home-use dialysis machine
Machine Features
Operator Controls
Display and backlight. Clinical dialysis machines commonly have relatively large displays (approximately the size of a computer screen), while home units have much smaller displays. Modern machines normally employ a graphical user interface (GUI) for ease of use. They use liquid-crystal displays (LCDs), instead of cathode ray tube (CRT) monitors, to reduce weight and power consumption.
Maxim supplies LVDS serializers and deserializers uniquely suited for LCD panels. These solutions cover a wide range of bit widths (from 1 to 27) and speeds up to 2.5Gbps. They can translate between different logic levels (e.g., from LVCMOS to LVDS) to ensure compatibility between the processor video interface and the display module.
A complete portfolio of products is available to equalize, multiplex, buffer, and level translate these interfaces as needed to ensure signal integrity. For example, the MAX3803 can equalize LVDS, PECL, or CML signals up to 3.2Gbps to compensate for as much as 40in of FR4 board material, thus ensuring the proper display of data in systems where the display is located far from the graphics processor.
Backlighting is required using either cold-cathode fluorescent lamps (CCFLs) or high-brightness white LEDs. Maxim provides drivers for both types of backlights. Available features include spread-spectrum clocking to reduce electromagnetic interference (EMI) and wide dimming ratios to support a range of ambient lighting situations. With the use of Maxim's ambient light sensors such MAX44009, which has human eye response, the display brightness can be controlled by a closed loop system to automatically adjust it to changing lighting conditions.
Touch screens and keyboards. Maxim offers a variety of keyboard scanners, including devices that allow multiple simultaneous key presses. In many applications, keyboards are being displaced by touch screens, which can improve the user experience when paired with an intuitive GUI.
In touch-screen applications, designers must consider the tradeoffs of using resistive vs. capacitive touch screens. If multiple touches are to be allowed, then capacitive touch screens are needed. If only single-touch inputs are required, the resistive approach has several advantages. For example, resistive touch screens are compelling for cost reasons in displays that are larger than a few inches. Maxim has several newer and smarter touchscreen controllers for both resistive and capacitive types that perform touch-management functions to reduce the burden on the processor managing this interface.
Patient Connections
For basic dialysis, there are no electrical connections to the patient. However, some dialysis machines monitor vital signs such as heart rate, temperature, and respiration rate, in addition to the patient's blood pressure. Since these functions are not specific to the dialysis process, they will not be discussed further in this application note.
Data Interfaces
A running record of the dialysis process for each patient session is kept electronically and made available in a number of ways. Dialysis machines can include USB, Ethernet, and a variety of serial (RS-232, RS-485, RS-422, etc.) interfaces to legacy hospital information systems. Wireless interfaces (such as Wi-Fi®) may also be included for direct connection to hospital wireless networks.
Data card slots are also available on some designs. This allows patients to carry an ID card with personal medical information stored on it to enable automatic setup of many of the machine parameters.
Mechanism
Pumps. Peristaltic pumps are commonly used for driving the various higher volume fluids in the machine: blood, dialysate, water, and saline. This type of pump is very convenient because it does not touch the fluids directly. Instead, a section of flexible tubing runs through the pump mechanism where it is compressed by rollers to push the fluid forward. These pumps require a significant amount of power and are driven by either DC or AC motors with variable speed control. Electronic means must be provided to ensure that the motor is turning at the desired rate. Maxim has Hall-effect sensors that give a fully independent signal picked up from actual shaft rotation, which can be used for redundancy if the motors already have Hall-effect sensors built in. For the lower volume fluids such as heparin, a syringe pump mechanism is commonly used driven by a small stepper motor or DC motor. Precise measurement of proper mechanism advance is needed.
Valves. Several valves with electronic actuation are needed in the machine to allow variable mixing ratios. Various implementations are possible from simple opened/closed valves driven by solenoids to precision variable-position valves driven by stepper motors or other means.
Sensors. Dialysis machines require many different types of sensors to monitor various parameters. Blood pressure at various points in the extracorporeal circuit, dialysate pressure, temperature, O2 saturation, motor speed, dialyzer membrane pressure gradient, and air are all monitored for proper values during dialysis. Unless they have digital outputs, the sensors' analog signals must be amplified, filtered, and digitized before being sent to the controller. The sensors require a range of ADC resolutions depending on the criticality of their accuracy, and a range of sampling speeds depending on the response times required.
Cleaning system. Between patient sessions, any reused components must be sterilized. One approach is to heat water or saline to a high sterilizing temperature and then run it through the machine, both through the extracorporeal circuit and through the dialysate circuit. Whatever cleaning mode is used, the machine may require additional driving and monitoring for proper operation.
Processing
Microcontrollers. Because of the large number of input signals to be monitored and the large number of pumps and other mechanisms to be controlled, many of these functions are performed with dedicated microcontrollers for that portion of the system. Controlling the overall system will be a main processor capable of running a full operating system and GUI. Communication between the controllers is required to send data, commands, and alerts.
Fail-safe circuitry. ICs with self-test and fault-reporting capabilities are very useful for maintaining patient safety under single-fault conditions. Additional monitoring circuitry is commonly used to monitor power-supply voltages, while watchdog circuits are used to ensure that microprocessor operation remains within bounds. Both audible and visible alarms are provided to alert users when a warning is needed or a fault condition has occurred.
Power Supply
Due to the long duration of the dialysis process, all dialysis equipment is AC-line powered. Standard AC-DC converters meeting medical safety standards are employed. Due to the variety of components requiring power, a variety of voltage rails are needed at different power levels. A power system with multiple-output switching regulators is needed with a significant amount of linear regulation at the load for noise-sensitive precision circuits.
Safety regulations require power-supply self-monitoring for voltage, temperature, and current flow.
Overvoltage and undervoltage detectors are common. Due to the higher power levels, active cooling is required using fans and temperature sensors in a variety of locations.
Home-use machines include water sterilization capabilities, which can require more power than is available from a standard wall outlet at 15A. Therefore, the power supply must be capable of limiting the current drawn from the AC line and adding in parallel power from a battery (or ultracapacitor).
Battery Management
As discussed above, home-use dialysis machines need to include batteries (or ultracapacitors) to supplement the power supply's output power when heating water for sterilization. These must be charged whenever possible and fuel gauged to indicate when enough capacity is available to proceed with the water sterilization process.